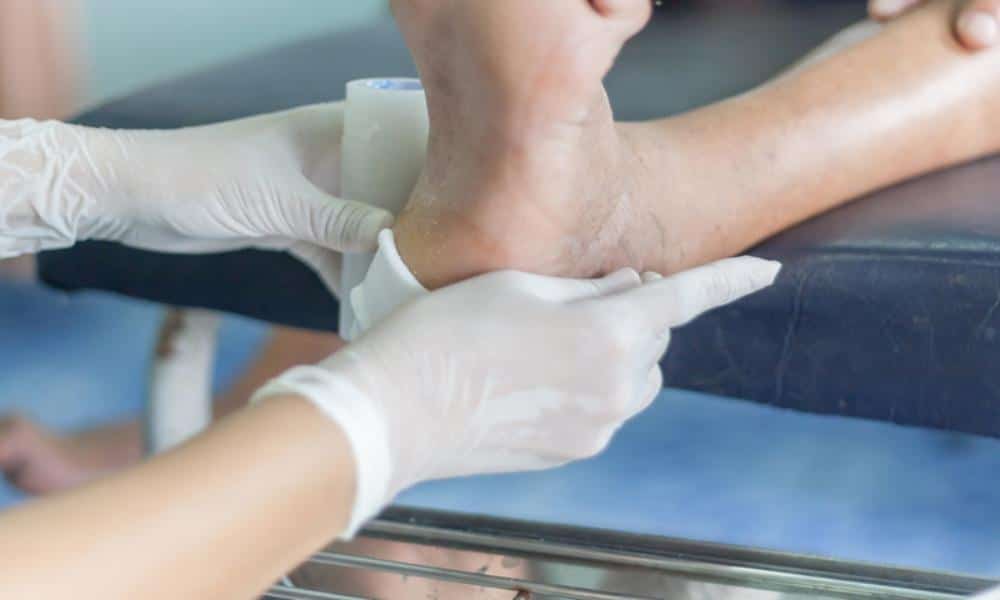
Diabetic ulcers on the foot can affect people with both type 1 and type 2 diabetes, occurring when the skin breaks down and skin layers beneath become exposed. These slow-healing wounds can become a serious health issue because they carry a high risk of infection, which may spread to the bone. Generally, antibiotics are effective, but if too much bone has been destroyed, it will have to be removed. According to the International Diabetes Federation, every 30 seconds, someone loses a lower limb or part of a lower limb because of diabetes.
Research suggests that 19% to 34% of people with diabetes will develop a foot ulcer at some point in their life. There are several types and knowing the differences between them helps podiatrists and doctors determine the right treatments.
Neuropathic Ulcers
Nerve damage (neuropathy) is one of the long-term complications of diabetes. It affects the nerves that carry touch, temperature and pain messages, especially nerves in the feet and legs. Neuropathic ulcers on the foot are caused by trauma or pressure which goes undetected due to a lack of sensation around pressure points. Calluses form at these sites and become so thick they traumatize the area beneath, causing ulceration. Minor cuts and scrapes also go undetected and therefore untreated and can eventually lead to the formation of ulcers.
Common sites of neuropathic ulcers: Pressure areas of the foot, such as the tips of toes, under the big toe and the sides of the foot and heel.
Appearance: Neuropathic ulcers are often round and have thick calluses on the surrounding skin. The depth of the wound depends on how much trauma the skin has been subjected to.
Ischemic Ulcers
Ischemic means reduced blood flow to a part of the body, and poor blood flow to the legs and feet damages tissue and causes cells to die. Ischemic ulcers occur when there is insufficient blood flow due to peripheral artery disease (PAD), an abnormal narrowing of the arteries. These diabetic ulcers are slow to heal and prone to rapid deterioration.
Common sites of ischemic ulcers: Toes, heels and the margins of feet.
Appearance: They can appear as pink, shallow open lesions with surrounding pink tissue. If the ulcer has dried up, there can be a black necrotic scab.
Neuroischemic Ulcers
These foot ulcers occur in people who have both peripheral neuropathy and ischemia resulting from peripheral artery disease. Neuroischemic ulcers are least likely to heal without intervention and, if infected, the risk of amputation is high.
Common sites of neuroischemic ulcers: Toes, margins of the foot and the dorsum of the foot. This is the part facing upward when a person is standing up. Neuroischemic ulcers can also develop on the tips of toes and beneath overly thick toenails.
Appearance: Pale or yellow-colored tissue that may have a halo of thin glassy callused skin. There can also be raised edges around the wound.
How to prevent diabetic ulcers on the foot
While diabetic ulcers are a common problem, they are preventable. Here are a few tips on how you can avoid them:
- The best offense is having a good defense. Therefore, if you have diabetes, you should inspect your feet daily and know how to recognize a problem before it becomes a significant issue. If you cannot examine your own feet, get a family member or carer to perform the task.
- Clean your feet daily and make sure to dry thoroughly between the toes. Apply moisturizer to prevent the formation of cracks.
- If you detect minor foot wounds such as cuts, clean them immediately and apply a topical antiseptic.
- Wear the proper footwear. Ill-fitting shoes can increase the risk of blisters which can turn into ulcers.
- Don’t walk around barefoot, especially if you have diabetic neuropathy.
- See a doctor immediately if you are experiencing abnormal symptoms such as fever, severe pain, redness or heat in the foot or pus coming out of a wound.
- Ensure toenails are trimmed straight across, while ingrown toenails should be treated promptly. If you can’t perform nail care, engage the services of someone trained in the care of diabetic feet.
How MINT can help you
If you have diabetic foot ulcers or think you may have, book an appointment with Dr. Akinwande and the Midwest Institute for Non-Surgical Therapy team. Our expert and friendly podiatrists will provide you with the right kind of treatment for your ulcers. We’ll also give you the know-how to take good care of your feet to prevent a recurrence of the problem.
We look forward to seeing you at one of our 5 convenient treatment locations in the St Louis MO and IL area, including Chicago.