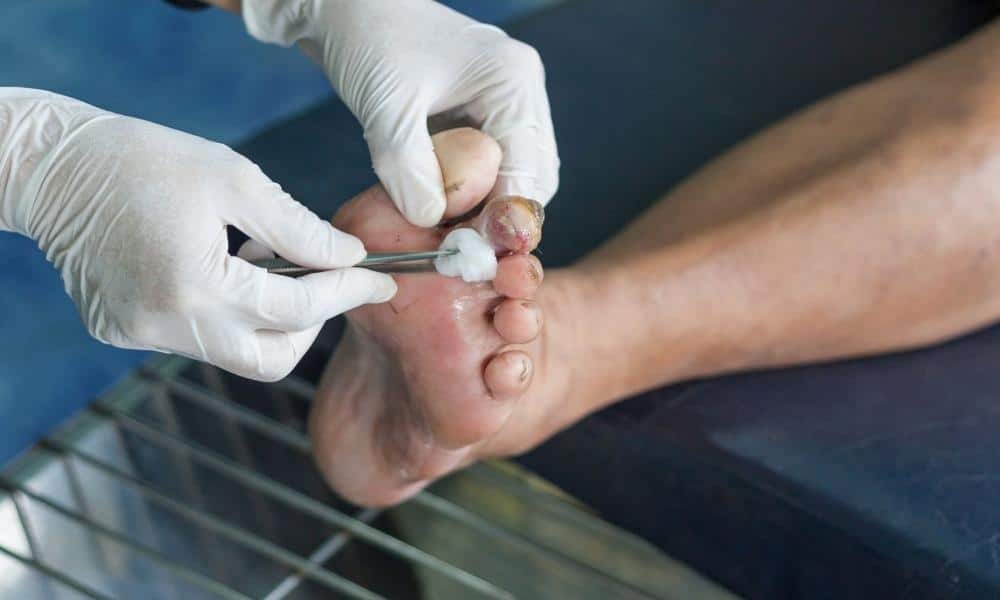
Amputation is one of the most feared complications of diabetes. Often it involves removing toes, feet and lower legs. The problems typically start in the feet with calluses that may progress to ulcers and complicated wound infections. Amputation is commonly needed if gangrene sets in, damage to the lower extremities is irreparable, or infections spread to the bone and cannot be stopped.
People with diabetes tend to be at a higher risk of amputations because high blood sugar levels over a long period can lead to poor circulation and nerve damage. Approximately 130,000 diabetes-related amputations occur every year in the USA, according to the National Institute of Diabetes and Digestive and Kidney Diseases. However, while the risk is more significant in people with diabetes, amputations are preventable in most cases, with both patients and clinicians playing critical roles in protecting limbs and extremities.
The Role of the Patient in Amputation Prevention
The best way to prevent amputation if you’re a person living with diabetes is to be proactive with your care. Each time you see your healthcare providers, ask them to assess your risk levels for developing ulcers or other complications. The sooner they are identified, the sooner they can be addressed. There is also a lot you can do to reduce the risk of problems that can lead to amputations.
Adopt a Healthy Lifestyle
Be aware of the inherent risks of smoking and alcohol in raising cholesterol and blood glucose levels and increasing your risk of developing foot complications. Managing blood sugar is essential. There are several ways to do this, including:
- Reducing stress
- Exercising for at least 30 minutes daily
- Eating a healthy diet of fruits, lean meats, whole grains, vegetables and fibers
- Regularly checking your blood sugar levels
- Taking your insulin and other medications as directed by your doctor
- Maintaining a healthy weight
- Quitting smoking if you are a smoker
Check Your Feet Daily
Perform daily foot inspections or have someone assist you if you’re unable to do this yourself. This entails:
- Examining the area between the toes and on the sides and bottom of the feet for cuts, bruises, cracks and broken skin
- Checking your nails for color changes, irregular edges and tears, and looking at the nail bed for signs of bruising or trauma
- Checking your shoes for foreign objects before putting them on
- Using an infrared thermometer to check the temperature of your feet. Temperature changes may be an early warning sign of complications
Additionally, every person with diabetes should have an annual foot inspection with a healthcare professional at least once a year or more if they’re at a higher risk of foot complications.
Seek Treatment For Foot Complications
If you have a wound or other foot complications, seek help as soon as possible to stop the problem from getting worse and putting your foot or leg at greater risk of amputation.
Prevent Foot Ulcer Recurrence
If you’ve had a foot ulcer and it has healed, the chances of a recurrence are reasonably high. One of the reasons is the new tissue is not as strong as the original. Therefore, continue with your daily foot and nail examinations, eat a healthy, balanced diet, manage blood glucose, blood pressure and cholesterol levels and wear comfortable shoes.
Deal with Diabetic Burnout
Diabetic burnout is where people can feel overwhelmed or frustrated by their diabetes and the stress of constantly having to pay attention to diet and other lifestyle factors. To recover, talk to your care team when things upset you, consider joining a support group to connect with other people and pamper yourself with a relaxing massage or long soak in the bath.
The Role of the Clinician in Amputation Prevention
Healthcare professionals also play critical roles in reducing the risk of amputation by ensuring appropriate and timely care. This includes considering making a health assessment that considers the whole patient, such as where they live, work and play and the type and quality of the support care they’re receiving.
Clinicians also manage active diabetic foot-related problems such as ulceration, neuropathy and bacterial, viral or fungal infections. This involves diagnosing the underlying problem, managing the treatment and preventing recurrence. Timely, expert care can save a limb and a life.
Final Thoughts
Amputation prevention for people with diabetes is a team effort involving healthcare providers such as doctors and nurses working closely with patients. At MINT’s vascular center, we focus on Peripheral Artery Disease (PAD), one of the leading causes of amputations. Our specialist treatments restore circulation by clearing blocked arteries. If you think you are at risk of PAD or amputations, call today to schedule an appointment at one of our 5 clinics, including the latest addition in Chicago, IL.