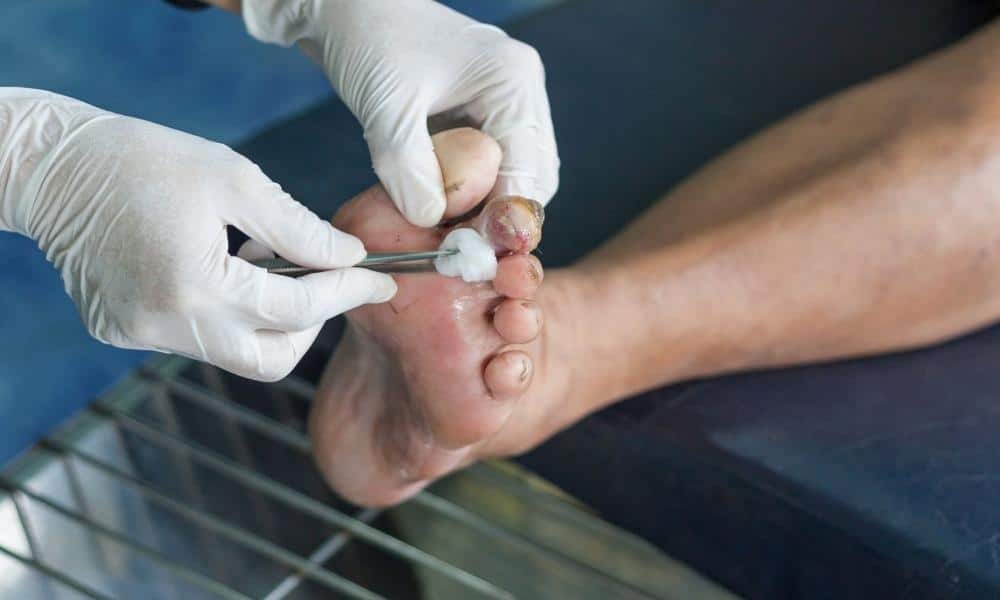
A diabetic ulcer on the foot is a break in the two top layers of skin, the epidermis and dermis, but it may also extend more deeply to the tendons and even the bone. These open wounds occur in approximately 15% of people with diabetes, according to the American Podiatric Medical Association. They are among the most common complications of diabetes and are responsible for more hospital admissions than any other.
Diabetic foot ulcers can appear anywhere below the ankle on the feet or toes. However, typically they develop in areas that encounter repetitive trauma and pressure, such as the bottom of the foot. An ulcer on the ankle is not classified as a diabetic ulcer on the foot.
Often people are unaware of the presence of an ulcer until they notice a yellow, brown or red drainage fluid on their socks.
There are numerous factors that increase a person´s risk of getting a diabetic ulcer on the foot. They are:
Uncontrolled Blood Sugar Levels
High blood sugar levels cause nerve damage, especially in the lower legs. This diabetic neuropathy prevents people from feeling cuts, blisters, sores or other damage to their feet. If these wounds go unnoticed and therefore untreated, they can develop into severe ulcers.
Poor Blood Flow
Peripheral artery disease (PAD) occurs when one or more arteries supplying blood to the legs and feet become blocked, impeding the flow of blood. Reduced blood flow means fewer germ-fighting cells getting to the feet to fight infections.
An open wound creates an entry point for infection, and if it spreads and is not treated or doesn’t respond to treatment, amputation may be necessary.
A Foot Deformity
Higher-than-normal blood glucose levels can also damage the motor nerves controlling foot muscles. This can lead to a foot deformity that develops into an ulcer or open wound.
A foot deformity known as hammertoe (where a toe is bent because of joint deformities) also increases risk. If an affected toe repeatedly rubs against a shoe, the skin will break down, which can lead to a foot ulcer.
Diabetic Complications
People with diabetic complications such as retinopathy (damage to the retina of the eyes) and nephropathy (kidney disease) are also at a higher risk of having a foot ulcer and amputation.
Calluses on Feet
Calluses are areas of thickened skin that form as a result of pressure, friction or other types of irritation. Increased skin temperature (hotspot) at a callus site is a precursor of diabetic foot ulcers.
Recent Transplant Recipients
People with diabetes who have recently had transplants of the pancreas, kidney or kidney-pancreas combined are also at an increased risk of developing a diabetic ulcer on the foot.
Other Risk Factors
Other risk factors include obesity, smoking, diabetic kidney disease and previous foot ulceration. The support a person has and their ability to look after themselves can also be a significant risk factor. For example, an elderly person living on their own who cannot reach their feet may not be able to check them regularly, which puts them at a higher risk of developing an ulcer.
Recurrence of Diabetic Foot Ulcers
Recurrence is also a common problem. According to a research paper in the Journal of Clinical Orthopedics and Trauma, approximately 40% of people will have a recurrence within one year after the ulcer has healed, 60% within three years and 65% within five years. The main risk factors for the recurrence of diabetic foot ulcers among patients are:
- Smoking
- Duration of diabetes
- Peripheral artery disease
- Diabetic peripheral neuropathy
- Duration of past diabetic ulcers on the foot
Preventing Diabetic Foot Ulcers
The good news is that diabetic foot ulcers are preventable. The best way to prevent them is to manage blood glucose levels to prevent diabetic neuropathy and PAD.
Doctors also recommend daily foot inspections so that any injury can be addressed immediately to stop it from becoming an open sore. Other recommendations include:
- Losing weight if you’re obese. Being overweight puts stress on the feet, which can rub against shoes leading to cuts and blisters.
- Quitting smoking
- Wearing footwear that fits comfortably
If you have diabetic ulcers on your feet or are at an increased risk of developing them, contact the friendly and professional podiatrists at the Midwest Institute for Non-Surgical Therapy (MINT). We’ll examine your feet and, if treatment is needed, will create a customized plan for you. To make an initial consultation, use our online booking service today to visit one of our 5 clinics, including the latest addition in Chicago, IL.