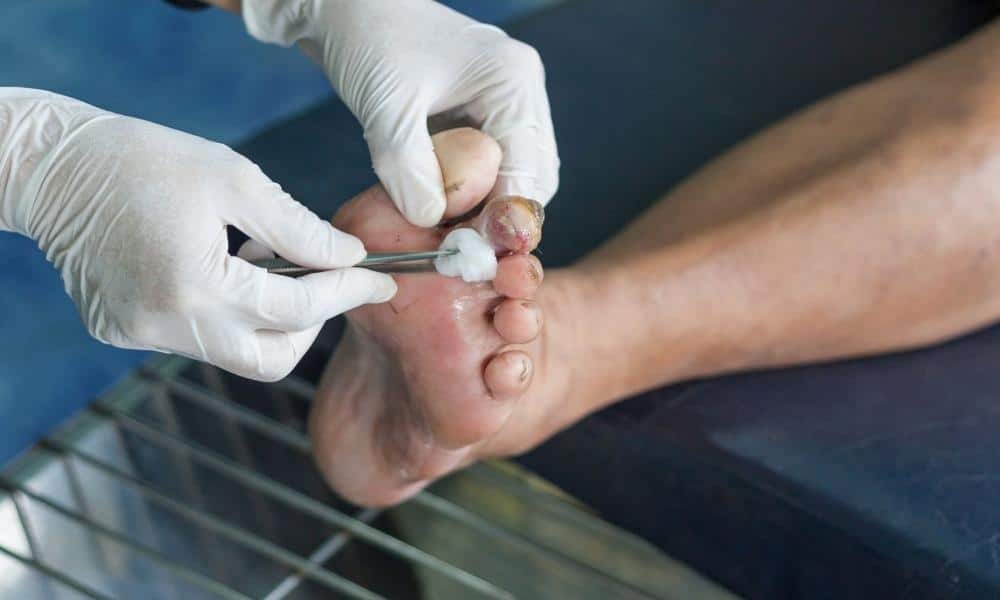
People with diabetes are at an increased risk of developing peripheral artery disease (PAD), a common circulatory problem caused by narrowing of the peripheral arteries (those that don’t supply blood to the heart and brain). This typically results in reduced blood flow to the head, arms, stomach and legs, causing such symptoms as leg pain when walking, sores on your toes and feet and painful cramping in the hips and thighs. Left untreated, peripheral artery disease can lead to stroke, heart attack and limb amputations.
According to figures from the American Diabetes Association, about 1 in 3 people with diabetes over the age of 50 have PAD.
The Diabetes and PAD Connection
PAD is similar to coronary artery disease, where arteries supplying blood to the heart become blocked. Except that PAD involves arteries leading to your extremities, often legs and feet. PAD develops when fatty deposits accumulate in the peripheral arteries causing them to narrow. This is also known as atherosclerosis or plaque build-up (fat, cholesterol and other substances) on artery walls.
The link between diabetes and peripheral artery disease is multifaceted, but people with diabetes are at a greater risk of developing atherosclerosis, which is the most common cause of PAD.
PAD and diabetes share several risk factors. These include:
- Being overweight or obese
- Sedentary behavior/lack of physical exercise
- High blood pressure (hypertension)
- High cholesterol
- Smoking
- Family history of coronary artery disease
PAD and diabetes also share a common complication, namely leg sores that are slow to heal. A possible explanation for this is that one condition may exacerbate the other.
People with diabetes who also have peripheral artery disease are at an increased risk of developing critical limb ischemia. This is a severe form of PAD and is a blockage in the arteries of the lower extremities that markedly reduces blood flow. It leads to severe pain in the feet and toes, and untreated may result in amputation of the affected limb.
How is PAD Diagnosed?
Many people with PAD and diabetes do not have any symptoms. Some may experience mild leg pain, which they put down to getting older, but it could be a warning sign, especially if you have diabetes. Other symptoms can include hair loss on legs and feet, numbness or weakness in the legs, shiny skin, and leg muscles shrinking or wasting.
Some of the tests a medical professional may perform to diagnose PAD are:
A physical examination may detect PAD signs such as a weak pulse or poor wound healing in a part of your body where blood flow is restricted.
Ankle-brachial index: A standard test that compares the blood pressure in your arms with the blood pressure in your ankles. If it is lower in the lower parts of your legs than your arms, you may have PAD.
Angiography: Using a dye injected into your blood vessels, your doctor can trace its flow with imaging techniques such as X-rays and magnetic resonance angiography MRA. This helps to identify any abnormalities in your arteries.
Ultrasound: With ultrasound imaging techniques, a doctor can detect blocked or narrowed arteries.
Early Detection Is Vital
If you are experiencing any symptoms of PAD, early diagnosis and treatment matter. The longer you wait, the lower your chances of having minimally invasive treatments. You will also elevate your risk of serious complications that can lead to amputation.
PAD Treatments for People With Diabetes
Once diagnosed with peripheral artery disease, there are several steps you can take to manage the risk factors. Chief among these will be making lifestyle changes that can lower your risk for both PAD and diabetes. Lifestyle changes include losing weight, quitting smoking and maintaining a diet low in saturated fat to help lower cholesterol and blood pressure. Cholesterol and high blood pressure medications may also be prescribed.
Increasing your physical activity is also essential. However, due to any pain you may be experiencing, this may have to be a supervised exercise regime. It will probably start slowly with leg exercises and treadmill programs. Your doctor will also be able to help you develop an appropriate exercise plan you can do at home
In some cases, people with PAD and diabetes may need surgery. For example, an angioplasty, which involves inserting into an artery a small tube with a balloon attached. The balloon is inflated to widen the blood vessel, and a stent may be left in place to help keep it open. Another approach is an artery bypass where a blood vessel is taken from another part of the body and attached to bypass the blocked artery.
To help prevent PAD and improve PAD symptoms, the skilled and knowledgeable team at the Midwest Institute for Non-Surgical Therapy specializes in PAD screening and endovascular treatments. Why not schedule your free vascular screening or use our online booking service today to visit one of our 5 clinics, including the latest addition in Chicago, IL.