At a glance:
- Varicose veins often cause aching, heaviness, throbbing, itching, or swelling—especially after standing.
- Many people have venous reflux/venous insufficiency (“leaky vein valves”) underneath visible varicose veins.
- A venous ultrasound can help identify the cause and guide minimally invasive options.
- Seek urgent care for sudden one‑sided swelling, redness, severe pain, chest pain, or shortness of breath.
What This Symptom Can Mean
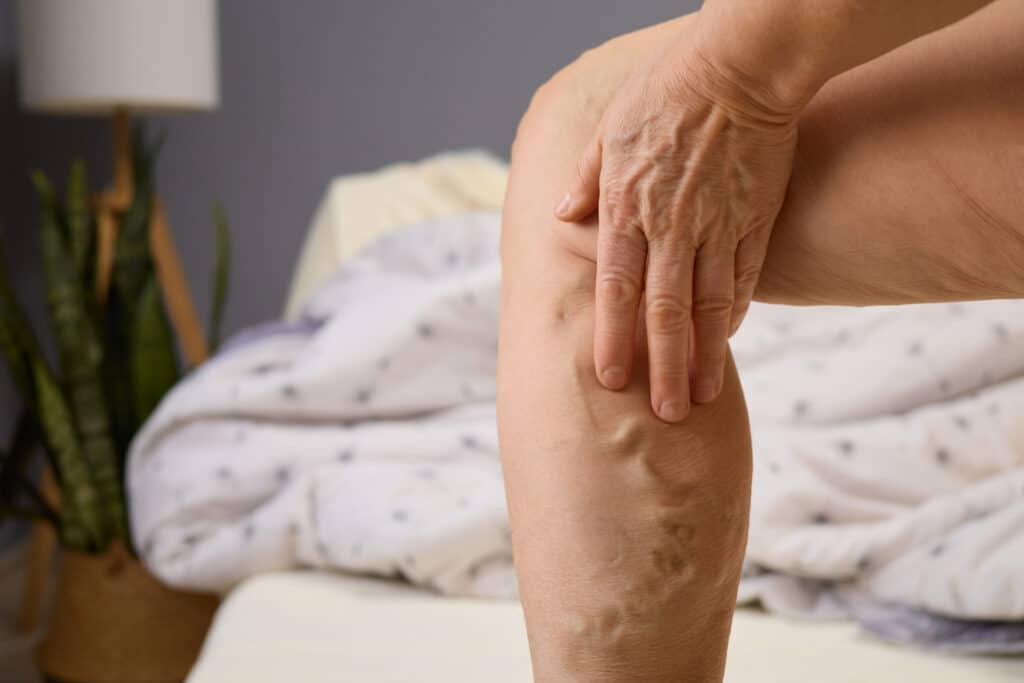
Varicose veins are enlarged, twisted veins that can appear as bulging “rope‑like” veins, usually in the legs. They may be primarily a comfort and quality‑of‑life issue, but they can also be a sign that the valves in the leg veins are not working well.
Common feelings patients describe:
- Aching
- Heaviness
- Tightness
- Throbbing
- Itching
- Restless legs
- Cramping
- Swelling that worsens later in the day.
Common Causes (In Plain Language)
A frequent driver is venous insufficiency (venous reflux)—when vein valves don’t close properly and blood falls backward, increasing pressure in the veins.
Some patients may also have issues deeper in the venous system (such as iliac vein compression/deep venous obstruction) that can contribute to swelling or recurrent symptoms.
Risk factors can include:
- Family history
- Pregnancy
- Prior blood clots
- Standing for long periods
- Age.
Quick Self-check
These questions can help you decide whether a vein evaluation is worthwhile:
- Do symptoms worsen after standing or sitting for long periods?
- Do you feel heaviness or aching that improves with leg elevation?
- Do you have visible bulging veins, ankle swelling, or skin color changes?
- Have you had a prior DVT/blood clot or leg vein procedure?
- Do you notice pelvic heaviness/pressure along with leg vein symptoms (could be related to pelvic veins)?
Red Flags: When to Seek Urgent or Emergency Care
Some symptoms can signal problems that need urgent evaluation.
- Call 911 or seek emergency care if you have chest pain or shortness of breath.
- Seek urgent medical care if you have sudden one‑sided leg swelling, significant redness/warmth, severe pain, or a new tender cord in the leg (possible clot).
- Seek urgent care for a rapidly worsening wound, fever, or spreading redness.
How We Evaluate Varicose Veins at MINT
We start with your symptoms and a focused exam, then usually recommend a venous reflux ultrasound to evaluate vein valve function and map the veins.
If symptoms suggest deeper venous involvement (for example, persistent one‑sided swelling or history of clot), we may discuss additional evaluation options.
- The goal is to identify the true source of symptoms, not just treat what’s visible.
Next Step: Request a Vein Evaluation
If you’re dealing with bulging veins, aching, heaviness, or swelling, the next step is a vein evaluation to confirm the cause and review options such as vein closure techniques and other minimally invasive treatments.
Medical information on this page is for general education and is not a substitute for personalized medical advice. If you believe you have an emergency, call 911.
FAQs
Are varicose veins dangerous or mostly cosmetic?
Many are not dangerous, but symptoms and skin changes can be meaningful. An evaluation helps determine if reflux or deeper venous issues are contributing.
What is venous insufficiency (venous reflux)?
It’s when vein valves don’t close properly, allowing blood to flow backward and raise pressure in the veins.
Do I need an ultrasound?
Ultrasound is commonly used to confirm reflux and guide the best treatment approach.
Can varicose veins come back after treatment?
They can in some cases, especially if underlying reflux or deeper venous issues persist—follow‑up and proper workup reduce recurrence.
What treatments do you offer?
Treatment options can include vein closure (ablation), medical adhesives (e.g., VenaSeal), foam therapy (e.g., Varithena), and other options depending on anatomy and evaluation.